MRIs May Provide More Accurate, Less Risky Prostate Cancer Screening and Diagnosis
By Joy Stephenson-Laws, J.D., Founder
As recently as a decade ago, the prostate-specific antigen (PSA) test was considered the gold-standard in front-line screening for possible prostate cancer. Doctors routinely recommended this test for their male patients over the age of 50 as well as for younger patients with risk factors such as a family history of prostate cancer or a genetic disposition to the disease. If the PSA test – either alone or in combination with a digital rectal exam - indicated a possible cancer, doctors would then order a biopsy to confirm whether cancer cells were present in the patient’s prostate. These results would then be used to determine if a course of treatment – such as surgery, chemotherapy, hormone therapy and radiation therapy – was indicated.
While this protocol may seem quite straightforward and even logical, the medical community’s experience has shown that it may present more risk than benefit to many patients. As a result, there is an ongoing disagreement as to the advisability of using the PSA as a screening tool for prostate cancer. Some physicians no longer recommend the test except in very specific situations, and others prefer to leave the decision to their patients’ “personal preference” based on their individual situations after weighing the benefits and risks of the test (which is the current recommendation of the U.S. Preventive Services Task Force).
And a biopsy procedure, which is required to confirm any cancer along with its grade (which describes how abnormal the cancer looks under a microscope and how quickly it is likely to grow and spread), has also come under greater scrutiny given that it carries a variety of risks of its own. These include pain, infection, difficulty urinating, bleeding at the biopsy site and even blood in the semen.

Just in case you may not be familiar with either the prostate or prostate cancer, a primer would be helpful before reading further. The prostate gland makes a fluid that both protects and nourishes a man’s sperm. It is about the size of a walnut and is located just in front of the rectum (which makes it easy for a doctor to examine by touch by inserting a finger into the rectum). Your risk for prostate cancer increases steadily as you age. It affects 1 in 39 men between the ages of 40 and 59, and 1 in 14 between the ages of 60 to 69. It is rare in men under the age of 40 (occurrence is 1 in 10,000, or .01%). According to the U.S. Centers for Disease Control and Prevention (CDC), prostate cancer is the most common cancer among men in the United States, other than non-melanoma skin cancer.
Why the current PSA-driven screening model has become controversialThe PSA test measures the amount of a very specific antigen in a man’s blood. In theory, the higher the amount of PSA, the greater the probability that he may have prostate cancer even if he has no physical symptoms. But an elevated PSA level can also be caused by a noncancerous condition. And, urinary tract infections, some medications and inflammation of the prostate (known as prostatitis) can cause changes in a man’s PSA levels.
Conversely, the lower the PSA in the blood, the less likely it is to have the probability of prostate cancer. The problem is that doctors and researchers have found that the levels of PSA in a man’s blood may not reflect the true probability of prostate cancer. What this means is that some men with high PSA levels may not have cancer (a higher number is normal for them) while others with low PSA levels may, in fact, have cancer. It also poorly differentiates between lethal and harmless prostate cancer. And further, it is not entirely clear if this screening saves lives.
To some in the healthcare community, the result of this uncertainty is that they believe the risk of a PSA may outweigh any benefit the test may offer. A patient with a high PSA test result, for example, may be counseled to undergo the inconvenience, cost and risks of a biopsy when it may not be necessary. And since a biopsy only takes samples, usually 10-12, of cells from different areas of the prostate it is possible that it could miss cancer cells should these samples only collect healthy cells. This could result in a false negative diagnosis. And, if the biopsy indicated no cancer, even if this is truly the case, having a high PSA level and a negative biopsy could still create stress for the patient over the incongruity of the two tests’ results.
Biopsies may also detect low-risk tumors that do not require treatment and that may be best left alone since the probability is that a man with them would succumb to other causes before he would to a slow growing, low risk tumor. But some doctors and mental health professionals may argue that having knowledge of the tumor – no matter how low the risk – may create enormous psychological strain for the patient. And in some situations, this knowledge may motivate a patient to ask for and/or undergo unnecessary cancer treatment that can carry its own health risks, including often debilitating and sometimes permanent side effects.
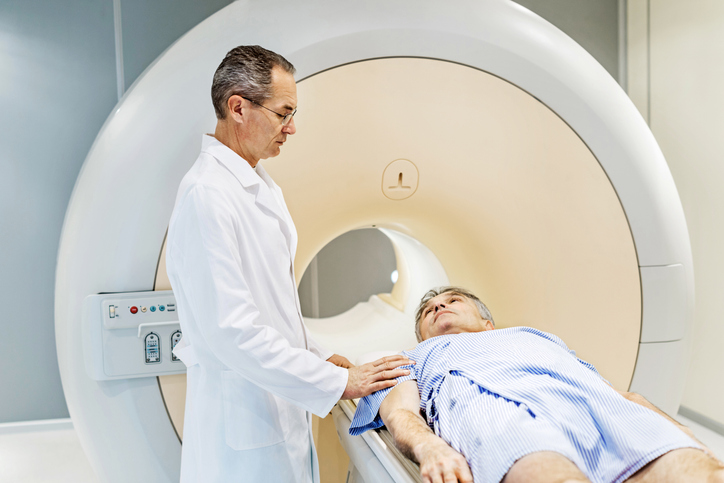
MRI may be a better screening toolUsing imaging technologies to help screen for cancer is not new. Women, for example, routinely are screened for breast cancer by having a mammography, a low-energy X-ray, which helps doctors examine breast tissue for indications of possible cancer. This is the same idea behind using MRIs in screening for prostate cancer. The MRI (which stands for Magnetic Resonance Imaging) uses strong magnetic fields and radio waves to generate very detailed images of the prostate gland itself. This allows physicians to examine the entire gland for possible cancer.
This approach to screening eliminates the uncertainty and inaccuracies inherent with a PSA test since the MRI allows the physician to “see” the prostate rather than rely on a blood marker that may indicate cancer. Should the MRI identify a possible area of concern, this area can then be further examined through a very targeted biopsy.
In one study, which appeared in the New England Journal of Medicine, this approach to screening and diagnosing prostate cancer was shown to potentially cut overdiagnosis of prostate cancer by half. According to researchers, it also holds the promise of reducing the number of unnecessary biopsies (which some estimates put at over a quarter of prostate biopsies) and the identification of minor, low-risk rumors without running the risk of missing clinically significant tumors.
What can you do to be proactive about prostate cancer?
Here are a few ways:
- Know the early symptoms. These symptoms include the following:
- Need to urinate frequently, especially at night
- Difficulty starting urination or holding back urine
- Weak or interrupted flow of urine
- Painful or burning urination
- Difficulty having an erection
- Painful ejaculation
- Blood in urine or semen
- Keep body fat in check. High body fat is associated with increased prostate cancer risk. This may be because body fat secretes hormones and specialized proteins that can increase inflammation and oxidation in the cells of your body. Inflammation and oxidation can lead to cancer. Reducing excess body fat is critical and not just for prostate cancer. Toxins love to make themselves at home in fatty tissue. The more fat, the more toxins you may carry in your body.
- Eat anti-inflammatory, antioxidant-packed foods. Many antioxidant and anti-inflammatory agents are found in colorful fruits, vegetables, whole grains, spices, and polyphenol-rich drinks such as pomegranate juice and green and black teas. Omega-3 fatty acids found in seafood contain anti-inflammatory properties that can also help reduce your prostate cancer risk.
- Munch on veggies with protective properties. Certain vegetables such as broccoli, Brussels sprouts, bok choy, wasabi and horseradish contain protective “phytochemicals” that may reduce your risk of prostate cancer.
- Get moving. Endurance exercises such as walking, running, cycling and swimming are particularly effective at increasing the body’s natural levels of antioxidants.
Since getting any type of medical screening is a very personal and important decision, you should talk with a competent medical professional about the benefits and risks of each, learn as much as you can about them and then make the best personal decision for you and your situation.
Enjoy your healthy life!
Disclaimer: This article is not intended to provide medical advice. Please consult with your doctor or another competent healthcare practitioner to get specific medical advice for your situation.
The pH professional health care team includes recognized experts from a variety of health care and related disciplines, including physicians, attorneys, nutritionists, nurses and certified fitness instructors. This team also includes the members of the pH Medical Advisory Board, which constantly monitors all pH programs, products and services. To learn more about the pH Medical Advisory Board, click here.







